Authors
Jill Christensen MD MPH Providence Milwaukie Hospital
Heidi Davis MSW Providence Milwaukie Hospital
Charlotte Navarre RN Providence Milwaukie Hospital
Hsin-Fang Li PHD Providence Medical Data Research Center
Kathy Schwab MPH RDN Providence Health Education
Richard O’Neil MBA Providence Planning Analyst
Title Diabetes Education with a Teaching Kitchen Intervention Can Improve Hemoglobin A1c for Type 2 Diabetics Compared to Traditional Diabetes Education
Purpose The Providence Milwaukie Community Teaching Kitchen offers health-focused, budget friendly cooking classes for patients. In 2019, we piloted diabetes education classes with an added hands-on culinary session. This study compares the change in hemoglobin A1c for patients who participated in the pilot with those in the standard curriculum and those referred to diabetes education but did not enroll.
Methods This retrospective analysis compared change in hemoglobin A1c for all patients referred to diabetes education in the Providence Northern Oregon region in 2019. Patients referred to diabetes education but not enrolled were considered a control group. To balance patient characteristics (e.g. age, gender, and pre-A1c score), two-to-one propensity score matching method was used to identify two matched controls for each enrollee. Change in hemoglobin A1c from baseline to 3-6 months were compared among matched comparison groups.
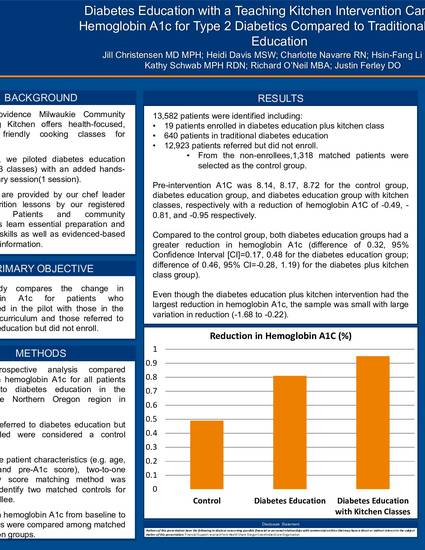
Results 13,582 patients were identified including 19 patients enrolled in diabetes education plus kitchen class, 640 patients in traditional diabetes education, and 12,923 patients referred but did not enroll. After matching, 1,318 matched patients were selected from the non-enrollees as the control group. The change in hemoglobin A1c was -0.49, -0.81, and -0.95 for the control group, diabetes education group, and diabetes education group with kitchen classes, respectively. Compared to the control group, both diabetes education groups had a greater reduction in hemoglobin A1c (difference of 0.32, 95% Confidence Interval [CI]=0.17, 0.48 for the diabetes education group; difference of 0.46, 95% CI=-0.28, 1.19) for the diabetes plus kitchen class group). Even though the diabetes education plus kitchen intervention had the largest reduction in hemoglobin A1c, the sample was small with large variation.
Conclusions Integrating a teaching kitchen component into the traditional diabetes education curriculum is a promising approach that can further improve initial biometric outcomes. Future studies are warranted to demonstrate clinical effectiveness of this enhanced intervention.
Financial Support Health Share Oregon Coordinated Care Organization
Available at: http://works.bepress.com/hsin-fang-li/8/
